Wednesday, February 27, 2008
7.25 Gee, I feel faint
In 1580, Geronimo Mercuriale formulated the concept of syncope and demonstrated that it was associated with a slow pulse rate: "Ubi pulsus sit rarus semper expectanda est syncope".
The precise cause of syncope, commonly known as fainting, is hard to pin down. The mechanisms, however, are quite well-known, for at least a few hundred years. Essentially, people faint because of a mixture of (1) cardiac inhibition from enhanced parasympathetic tone, and (2) vasodilation from sympathetic withdrawal. Simply put, a slowed heart rate that reduces blood flow to the brain thereby causing a patient to faint.
Like migraine headaches, there are many triggers for syncope - officially "vasovagal syncope", for example, stress, standing upright for too long [known to happen to the Guards at the Buckingham Palace], pain, the sight of blood, hunger, prolonged hyperthermia, just to name a major few. For a few seconds, the patient feels light-headed, experiences nausea, sweating, ringing in the ears, and visual disturbances, before losing consciousness. The patient then keels over and this is when the injuries occur.
Feeling faint in an eye doctor's office? Of course that happens. This is often confused with feeling dizzy or having blackouts; both of which need to be neurologically evaluated. And it is not quite the "true syncope" but the "near syncope". In other words, the patient has all the signs and symptoms but stops short of passing out. This occurs usually from four activities: (1) contact tonometry (both applanation and indentation - the instruments must touch the cornea to get IOP readings); (2) first-time contact lens trial; (3) slit-lamp biomicroscopy; and (4) insertion of punctal plugs. In all situations, once the patient's eyes or eyelids are touched by the tip of the tonometer, by the doctor or an assistant when inserting a contact lens, or by the doctor's pulling down the patient's lower eyelid for a closer view of the palpebral conjunctiva or the puncta, usually at the slit-lamp, vasovagal reflex kicks in within minutes. Interestingly, most patients are young and healthy, possibly for the first time in their lives, their eyes are now manipulated by a stranger. The eyes/eyelids are indeed under some mechanical pressure albeit quite minor yet the physical reaction is quite dramatic.
First aid is to have the patient lie down while raising his/her feet or at least lower the head, so the brain can get back some much-needed blood.
Call an ambulance? Nah. The patient recovers on his/her own within minutes. Although it is not unheard of that a complete cardiac work-up is ordered if the patient ends up in the ER. And at least one patient brought a lawsuit against one eye doctor for some unspecified damages and emotional stress (remember: this is the United States of America, home to many personal injury barristers).
Some patients are disappointed that they probably won't be able to wear contacts, ever. Some are a bit embarrassed yet are quite happy to have a tale for their loved ones. Fortunately, vasovagal syncope, true or near, is never fatal.
Think about this: For patients with a history of having trouble instilling eyedrops or inserting contacts, it may not be a matter of dexterity but a mild form of vasovagal reaction.
Sunday, February 24, 2008
7.24 You have small eyes
Enough fun with the Singapore sling, now we move on to something intriguing.
Despite the outward appearance, all emmetropic and hyperopic eyeballs are pretty much the same in size. The myopic eyes are indeed a little bigger. And once in a while, we need to inform a patient, "You have small eyes." This is not being impolite, but to point out the presence of nanophthalmos (dwarf eye). Nanopthalmos is not to be confused with microphthalmia (small eye); the latter is a congenital malformation with other developmental issues, often from fetal alcohol syndrome or viral infection in utero. Patients with hereditary nanophthalmos may have a defective gene on Chromosome 11; otherwise, they are developmentally normal.
Nanophthalmos with uveal effusion is a nasty condition first described by Dr Robert Brockhurst of Boston, Massachusetts, in 1974. These patients often develop narrow-angle glaucoma that prompted surgical intervention. Unfortunately, this also results in secondary retinal and choroidal detachment - owing to uveal effusion. Further repair is ineffective and sometimes choroidal elevation can be mistaken as intraocular tumors. So the recognition of nanophthalmos is important in order to manage it correctly.
Maybe this is a good time to look at the size of human eyeballs. We have been able to convince some patients to volunteer for MR imaging of the eye:
| Type of Eye | Mean ± SD (diopter) | Range (diopter) |
| Nanophthalmos (phakic) | +10.42 ± 6.22 | +4.50 – +18.50 |
| Hyperopia | +3.42 ± 0.66 | +3.00 - +4.50 |
| Emmetropia | +0.21 ± 0.25 | -0.25 - +0.50 |
| Myopia | -10.25 ± 4.31 | -6.25 - -15.50 |
And from MR images, it is possible to calculate the size of the eyeballs in 3D:
| Type of Eye | Axial1 | Equatorial1 | Coronal(H) | Coronal(V) |
| Nanophthalmos | 18.1 ± 2.02 | 19.0 ± 2.62 | 19.3 ± 3.02 | 18.2 ± 2.52 |
| Hyperopia3 | 23.1 ± 1.0 | 24.1 ± 0.5 | 23.8 ± 0.3 | 23.3 ± 1.4 |
| Emmetropia | 22.9 ± 1.3 | 23.9 ± 1.2 | 23.9 ± 1.5 | 23.0 ± 1.9 |
| Myopia4 | 28.5 ± 1.0 | 27.1 ± 1.5 | 28.3 ± 0.5 | 27.4 ± 0.7 |
1The equatorial lengths are significantly greater than the axial lengths: paired t-test P=0.006 and 0.025 for emmetropia and hyperopia, respectively. For nanophthalmic eyes, P=0.1 and for myopia, P=0.2.
2Unpaired t-tests between nanophthalmos and emmetropia in all dimensions, P<0.02.
3No difference between hyperopia and emmetropia.
4Unpaired t-tests between myopia and emmetropia in all dimensions P<0.01.
Clearly, myopic eyes are big. And in contrast, nanophthalmic eyes are much smaller which is the hallmark of nanophthalmos.
If we look at the anterior segment closely:
Type of Eye | | Lens Thickness | Lens Diameter |
| Nanophthalmos | 3.0 ± 0.11 | 5.3 ± 0.82 | 8.5 ± 0.4 |
| Hyperopia3 | 3.1 ± 0.3 | 4.6 ± 0.6 | 8.7 ± 0.4 |
| Emmetropia | 3.0 ± 0.2 | 5.0 ± 0.8 | 8.4 ± 0.4 |
| Myopia4 | 2.6 ± 0.6 | 4.0 ± 0.3 | 9.4 ± 1.3 |
1Unpaired t-test when calculated as % axial length between nanophthalmos (16.5±2.5) and emmetropia (13.0±1.1): P=0.025.
2Unpaired t-test when calculated as % axial length between nanophthalmos (29.5±7.2) and emmetropia (21.7±2.9): P=0.06.
3No significant difference between hyperopia and emmetropia.
4No significant difference between emmetropia and myopia.
Table IV. Choroidal and scleral thickness (mean ± SD mm).
| | Axial | Vertical | Equatorial | |||
| Type of Eye | Choroid | Sclera | Choroid1 | Sclera | Choroid | Sclera2 |
| Naophthalmos | 0.7±0.3 | 0.7±0.3 | 0.7±0.3 | 0.5±0.2 | 0.6±0.3 | 0.7±0.3 |
| Hyperopia3 | 1.0±0.0 | 0.7±0.3 | 0.4±0.2 | 0.4±0.2 | 0.5±0.3 | 0.4±0.3 |
| Emmetropia | 0.9±0.2 | 0.6±0.3 | 0.5±0.1 | 0.4±0.2 | 0.5±0.2 | 0.4±0.2 |
| Myopia4 | N.M. | N.M. | N.M. | N.M. | N.M. | N.M. |
1Unpaired t-test between nanophthalmos and emmetropia: P<0.09; when calculated as % of total vertical axial length, nanophthalmos (4.0±1.8) vs. emmetropia (1.9±0.5): P<0.04. 2Unpaired t-test between nanophthalmos and emmetropia: P<0.08; when calculated as % of total equatorial axial length, nanophthalmos (3.4±1.4) vs. emmetropia (1.6±0.5): P=0.03. 3No difference between hyperopia and emmetropia. 4N.M. - Not measurable. Thicknesses less than the in-plane resolution of 0.31mm.
Ah, so that's it: the equatorial sclera is the thickest in the nanopthalmic eyes. It is almost like all eyes are given the same amount of building materials. Smaller eyes are constructed with thicker walls while larger (myopic) eyes with thinner walls. Thick equatorial sclera chokes off blood circulation through the vortex veins (each eye has 4 or 6 of these). The only effective treatment for relieving high eye pressure is therefore sclerostomy around the base of the vortex veins.
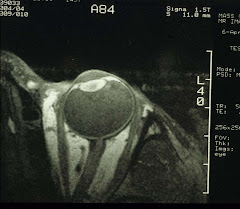
For those who have patiently read through the above, a bonus for you. We'll now show you how to perform high-resolution MRI of the eye (also the methodology used in the study described above):
MR imaging was conducted using General Electric 1.5 Tesla Signa body scanners. A home-made 1.25-inch receive-only surface coil tuned to the proton frequency of the imagers was placed over the eye of interest. [Note: the factory 3-inch TMJ coil also can be used.] The coil was constructed with variable capacitors that allowed tuning and matching. A sagittal head image series using an FOV of 20 mm or more was acquired to locate the eye. Slice selection in the axial plane was then determined using graphic prescription. Multi-slice images in the axial and coronal planes were obtained (usually 8-9 slices/plane/eye) using a T1-weighted spin-echo sequence with for example, TR/TE = 400/20 msec with an image resolution of 0.31 x 0.31 mm and a slice thickness of 3 mm (in this case, the image acquisition time was 4.5 min). Image slices was selected by aligning imaging planes as parallel to the antero-posterior axis as possible.