Most times, headaches can be diagnosed based on chief complaints, for example, in migraine and cluster headaches. One of the migraine prodromes, the occurrence of auras is quite well-known. [Note, however, in ocular migraines, auras do not lead to headaches.] And cluster headaches can last quite a few days; the patients often need to rest/recuperate in a dark and quiet place.
Patients with persistent headaches who show up in an eye doctor's office, are often referrals from the PCPs. The purpose is see if any of these apply: athenopia, angle-closure glaucoma, temporal arteritis, pseudotumor cerebri, pituitary tumor, etc. The PCPs may also plan, in addition to a complete physical to rule out hypertension, migraines, etc, neurological and radiological consults to ensure absence of space-occupying or vascular lesions, hemorrhages in the brain, or even meningitis. It is a multi-disciplinary process of elimination that can therefore be quite time-consuming.
From an eye doctor's perspective, any patients with headaches are suspected of having one of the following until proven otherwise:
Beyond the routine headaches checklist (throbbing/sharp/dull, where, when, how long, how bad, how treated), the first exam is to see if asthenopia is a contributing factor. Asthenopia is simply headaches caused by eye strain or uncorrected refractive error. The strain can occur when the eyes are forced to constantly re-focus, further worsened by insufficient accommodative reserve - typically in progressive hyperopia and/or incipient presbyopia, and much less well-known, in uncorrected astigmatism. The patient's complain of pain is usually vague; although it mostly refers to heaviness in and around the eyes. The symptoms disappear as soon as the refractive error is properly corrected. A good example is to switch from spherical equivalent to toric contact lenses for a full astigmatism correction. And the accommodative lag or insufficiency is remedied by applying more plus (or less minus) power. Asthenopia is, however, never truly debilitating, nor is it sight- or life-threatening.
Often the patient with acute angle-closure glaucoma attack ends up in the ER department of a hospital. Because the symptoms can include headaches, nausea, and vomiting. During attacks, the eyes show steamy corneas with limbal flush and often a distorted pupil as well (see image below):
 As in acute angle-closure, patients with chronic narrow-angle glaucoma often complain of "brow aches". The cause is a true increase of pressure in the eye that can be readily measured with a tonometer. At the slit-lamp, gonioscopy is also performed to assess the angle - to see if the aqueous drainage is dangerously obstructed. Both hypotensive agents and laser iridotomy maybe needed to normalize the IOP to get to the origin of this type of headaches and prevent the visual field loss.
As in acute angle-closure, patients with chronic narrow-angle glaucoma often complain of "brow aches". The cause is a true increase of pressure in the eye that can be readily measured with a tonometer. At the slit-lamp, gonioscopy is also performed to assess the angle - to see if the aqueous drainage is dangerously obstructed. Both hypotensive agents and laser iridotomy maybe needed to normalize the IOP to get to the origin of this type of headaches and prevent the visual field loss.Temporal arteritis usually afflicts the elderly. It is a manifestation of a systemic giant cell arteritis that can sometimes lead to death. Usually the inflamed temporal artery can be seen snaking under the skin (shown in image below). The temple area is quite tender, certainly sensitive to touch, and painful while chewing. The blood supply to the optic nerve and the retina also can be compromised, causing irreversible loss of vision. Definitive diagnosis is based on erythrocyte sedimentation rate (ESR) and temporal artery biopsy. The treatment of choice is naturally the use of systemic steroids which can reduce the inflammation rather quickly.
 Then we have the pseudotumor cerebri. As the name indicates, this is not a real tumor inside the cranium, but an increase in intracranial pressure owing to the presence of excess cerebrospinal fluid (CSF). Usually the patient is a slightly over-weight woman of child-bearing age. Birth control pills, vitamin A, and tetracyclines are all risk factors. Because of the increase in the intracranial pressure as in hypertension, sometimes papilledema is seen (shown below). Papilledema is a swelling of the optic disc, so the disc margin is now raised and the demarcation blurred. These can be seen very easily with a hand-held ophthalmoscope.
Then we have the pseudotumor cerebri. As the name indicates, this is not a real tumor inside the cranium, but an increase in intracranial pressure owing to the presence of excess cerebrospinal fluid (CSF). Usually the patient is a slightly over-weight woman of child-bearing age. Birth control pills, vitamin A, and tetracyclines are all risk factors. Because of the increase in the intracranial pressure as in hypertension, sometimes papilledema is seen (shown below). Papilledema is a swelling of the optic disc, so the disc margin is now raised and the demarcation blurred. These can be seen very easily with a hand-held ophthalmoscope. Definitive diagnosis is lumbar puncture together with neuro-imaging, the latter to rule out brain tumor. There are other visual disturbances such as blurred vision and diplopia. In fact, these visual symptoms are the reason why the patients are referred to the eye doctors in the first place.
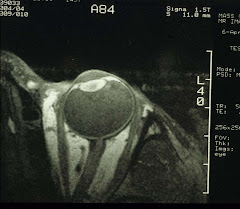
Definitive diagnosis is lumbar puncture together with neuro-imaging, the latter to rule out brain tumor. There are other visual disturbances such as blurred vision and diplopia. In fact, these visual symptoms are the reason why the patients are referred to the eye doctors in the first place.Speaking of brain tumor, pituitary adenomas that impinge upon the optic chiasm can cause bilateral hemifield loss. Which can be picked up by performing simple confrontation visual field tests. Definitive diagnosis is brain MRI. The MR image below is a T1-weighted coronal scan showing a large hyperintense area (arrows), i.e., the pituitary tumor.
 Headaches are of course a prominent feature of pituitary adenoma. They also can be the only manifest, and to the surprise of many eye doctors, without involving any visual field loss. Needless to say, pituitary tumors must be removed (usually through the nose to reach the base of the brain where the pituitary gland is).
Headaches are of course a prominent feature of pituitary adenoma. They also can be the only manifest, and to the surprise of many eye doctors, without involving any visual field loss. Needless to say, pituitary tumors must be removed (usually through the nose to reach the base of the brain where the pituitary gland is).Diagnosis and treatment of headaches can be exciting and rewarding - particularly if a potentially sight- and/or life-threatening lesion is the root cause. Fortunately, most cases are benign, stress-induced variety.